291:
be achieved with minimal risk of damage to the joint surfaces. Most surgeons will inject fluid into the joint at this stage, again to ensure that there is enough space between the ball and socket for safe instrument access. This needle is then removed. The next step is placement of the 'portals', or the small holes made to pass instruments into the joint. This is achieved by again passing a fresh hollow needle into the joint under x-ray control, usually in a slightly different position. The reason for this is so the surgeon can ensure that the needle, and subsequent cannulae do not penetrate and damage the acetabular labrum or cartilage joint surfaces (see fig. 5). Again, surgeons will have their own preferences as to their preferred placement. Through this hollow needle, a long thin flexible guide wire is passed into the joint, and the needle is removed over it, leaving the guide wire in situ. A small cut in the skin is made around the wire, to allow for larger cannulae to be placed over the wire through the portal. The wire therefore guides the larger cannulae into the joint. The most common external diameters of cannulae used are between 4.5 and 5.5 mm. Once the surgeon is satisfied that the cannula is in the correct position, by a combination of feel and x-ray guidance, the guide wire can be withdrawn. Once the first portal is correctly placed, any further portals may be created once the camera is in position, to ensure that they are placed with minimal risk to the joint surfaces. This process can be repeated to gain as many points of entry to the hip joint as the surgeon requires, normally between two and four. Certain of these entry points will be used for the viewing arthroscope and others for operating instruments.
253:
241:
265:
26:
140:
352:
contact pressures of the femur to the acetabulum. The labrum has also been shown to have a nerve supply and as such may cause pain if damaged. The underside of the labrum is continuous with the acetabular articular cartilage so any compressive forces that affect the labrum may also cause articular cartilage damage, particularly at the junction between the two, the chondrolabral junction. The labrum may be damaged or torn as part of an underlying process, such as FAI or dysplasia (shallow hip socket), or may be injured directly by a traumatic event. Depending on the type of tear, the labrum may be either trimmed (debrided) or repaired. Removing or debriding the labrum is becoming less popular as the latest research shows that results are more predictable in the long term if the labrum can be repaired. Various techniques are available for labral repair, mainly using anchors, which may be used to re-stabilise the labrum against the underlying bone, allowing it to heal in position.
415:
gain safe access to the joint. The most common nerve to be injured is the lateral cutaneous nerve of the thigh. This nerve supplies feeling to the upper, outer thigh. Other nerves that may be affected are the sciatic (leading to a weakness lifting the foot – 'foot-drop'), femoral (weak thigh muscles), obturator (numbness in the inner thigh and weakness of those muscles), and pudendal nerves. The pudendal nerves supply feeling to the reproductive organs. Persistent inflammation to the soft tissue structures around the hip after hip arthroscopy is not uncommon. This is usually self-limiting and improves with time, although occasionally requires anti-inflammatory treatment. The most commonly affected area is around the outside of the hip (greater trochanter), although inflammation of iliopsoas (the muscle which passes directly over the front of the hip) can also occur.
308:
132:
316:
junction (see fig. 6). The head-neck junction is at the base of the ball of the hip, where it joins the short neck, which in turn carries on downwards into the femur, or thighbone, itself. A bony protrusion or bump at the head-neck junction has been likened to a cam, an eccentric part of a rotating device. This leads to joint damage as a result of the non-spherical femoral head being forced into the acetabulum mainly with flexion and/or internal rotation. This may impart compression and shear forces to the articular cartilage, and may lead to labral tears and peeling away of the articular cartilage from the underlying bone, so-called cartilage delamination (see fig. 8).
107:
flip' approach to gain access to the hip joint. This is an extensive approach, needing an often large incision over the side of the hip, with the detachment of the greater trochanter of the femur and its attached musculature to gain access to the joint. By using this approach, the ball of the hip joint can be rotated out of the socket (termed 'surgical dislocation'), giving 360-degree access to the whole joint. This approach, although considered generally safe, carries with it inherent risks, which is the case with all large incision surgery. The risks of infection and blood clots are always present, and Ganz and his colleagues cite complications such as
283:. There are two widely used methods, one with the patient on their back (supine) and the other on their side (lateral decubitus). Which is used is down to the surgeon's preference. To gain access to the central compartment of the hip joint (between the ball and socket), traction is applied to the affected leg after placing the foot into a special boot. (See fig. 2) There is specifically designed equipment for this, although some surgeons use a 'traction table', initially designed to help in the operative fixation of broken thigh and lower leg bones. The amount of traction (or pull) needed is assessed with the help of
78:(hip) joint through an arthroscope and the treatment of hip pathology through a minimally invasive approach. This technique is sometimes used to help in the treatment of various joint disorders and has gained popularity because of the small incisions used and shorter recovery times when compared with conventional surgical techniques (sometimes referred to as "open surgery"). Hip arthroscopy was not feasible until recently, new technology in both the tools used and the ability to distract the hip joint has led to a recent surge in the ability to do hip arthroscopy and the popularity of it.
450:
119:) in the hip joint, and a small risk of damage of the blood supply to the femoral head. The patient usually needs to stay in hospital for a few days, and the post-operative rehabilitation after such extensive surgery can be prolonged. As a result, surgeons have looked to use the arthroscope more extensively in the hip joint in an attempt to avoid the possible pitfalls of large, open surgery. The perceived advantages of this are the avoidance of large scars, decreased blood loss, faster recovery periods and less pain. Hip arthroscopy can be performed as an
329:
the rim. This results in contact of the femoral neck against the labrum and rim of the acetabulum during hip movement earlier than might otherwise be the case. Repeated contact between the femoral neck and the edge of the acetabulum may lead to damage to the labrum and adjacent articular cartilage. Bone formation, or ossification within the labrum may be commonly seen as a result of this repeated contact. It is thought that this type of impingement may also predispose to the development of
479:. The ligaments that keep the hip joint in place are in fact, thickened areas of joint capsule, rather than distinct structures. The synovium generates fluid that lubricates the joint; in that fluid are the nutrients needed to keep the cartilage cells alive. A total of 27 muscles cross the hip joint, making it a very deep part of the body for arthroscopic access. This is one reason why hip arthroscopy can be quite technically demanding.
264:
475:, a fibrous structure that envelops the femoral head. (See fig. 1) The labrum acts as a seal, or gasket, around the femoral head. However, this is not its only function, as it has been shown to contain nerve endings, which may cause pain if damaged. The blood supply of the labrum has also been demonstrated. The joint itself is encompassed by a thick, fibrous joint capsule, which is lined by
252:
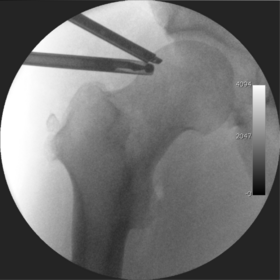
287:(low-dose portable x-ray). (See fig. 3) It is usually not possible to distract the ball from the socket with traction alone by more than a few millimetres. Once the surgeon is happy that they will be able to gain access to the hip joint (i.e. the ball will distract from the socket by a small amount), the patient is then painted with antiseptic and the surgical drapes applied.
428:
encouragement for a free range of movement, stretches and isometric exercises leading to subsequent dynamic, plyometric and weights exercises. Impact activities are usually discouraged for a minimum of three months, and contact sports for four. Using a simple stationery pedal device the first day after surgery can be key to immediate flexibility and mobility after surgery.
483:
ligamentum teres carries a blood vessel from the pelvis to the femoral head. This blood vessel usually becomes redundant with age. Arthroscopic hip surgeons are becoming increasingly convinced that the ligamentum teres acts as an internal stabiliser of the hip joint, and pathological injury to the ligament is now a recognised cause of hip pain and instability.
298:
Commonly used arthroscopic tools are the hook probe, used to assess the integrity and consistency of the hip, radiofrequency probes that ablate soft tissue and can also smoothen tissue surfaces, and various shavers or burrs that can take away diseased tissue. If the acetabular labrum requires repair,
290:
The next step is to insert a fine needle under x-ray guidance into the hip joint. This breaks the 'suction seal' of the joint and allows further distraction if necessary (see fig 4). The surgeon wishes to see the ball move out the socket by approximately 1 cm, so that access to the hip joint can
414:
Damage to nerves around the hip joint can occur, sometimes because of direct damage with the surgical instruments, or as a result of the traction needed to gain access to the joint. For this reason, surgeons prefer to apply as little traction as possible, for as short a time as possible, in order to
337:
the end of the procedure. With the exception of cases of severe global over coverage of the hip, or situations in which the existing labrum has turned to bone (or ossified), excessive acetabular rim resection should be avoided in order to prevent iatrogenic increases in hip joint contact pressures.
328:
In contrast, pincer impingement is a result of an abnormality on the acetabular side of the hip joint. The acetabulum may either have a more posterior orientation than normal, otherwise known as acetabular retroversion (seen as the crossover sign on AP radiographs), or there may be extra bone around
147:
Hip arthroscopy was initially used for the diagnosis of unexplained hip pain, but is now widely used in the treatment of conditions both in and outside the hip joint itself. The most common indication is for the treatment of FAI (femoral acetabular impingement) and its associated pathologies such as
94:
Arthroscopic techniques have become an increasingly popular method of treating hip conditions. Although first described in the 1970s, since approximately 2000 the indications and numbers of hip arthroscopic procedures performed worldwide have expanded widely. This is due mainly to the identification
436:
The results of hip arthroscopic techniques will depend on the indication for the operation and perhaps also on the experience of the surgeon. Published reports are certainly encouraging, and the number of research papers reporting the results of hip arthroscopic surgery is increasing rapidly. As an
336:
The goal of the arthroscopic treatment of pincer impingement is to reduce the acetabular over coverage of the hip. Methods to reduce this over coverage of the ball by the socket include labral detachment or peel back, acetabular rim trimming using burrs, often reattaching the labrum with anchors at
294:
The operation then begins, a variety of instruments being used. While the surgeon views the interior of the hip joint through the arthroscope, other operating instruments are introduced through the other portals. Once the surgeon has completed the procedure needed between the ball and socket, often
90:
to see inside a joint was
Severin Nordentoft, from Denmark, in 1912. Since that time, the field of arthroscopy has evolved to encompass diagnostic and therapeutic procedures to many joints. Technical advances in instrument manufacture and optical technologies have, in part, made it possible for the
351:
The acetabular labrum is a fibrous structure, which surrounds the femoral head. It forms a seal to the hip joint, although its true function is poorly understood. Recent evidence has demonstrated that this hydraulic seal is vital for maintaining stability of the ball and socket joint and reducing
427:
Each surgeon will have their own preferred physiotherapy schedule. Many are on their individual websites. A variable period on crutches after hip arthroscopy is common although physiotherapy is seen by many to play a very significant part in post-operative recovery. The regime usually starts with
418:
As with all arthroscopic procedures, because the hip arthroscopy is undertaken with fluid in the joint, there is a risk that some can escape into the surrounding tissues during surgery and cause local swelling. Occasionally, this causes skin blistering. However, swelling usually resolves after 24
319:
Standard arthroscopic treatment of symptomatic cam FAI involves debridement (resection) or repair of any labral and chondral injuries in the central compartment of the hip, and subsequent reshaping of the head-neck junction of the upper femur (osteochondroplasty) in the peripheral compartment
315:
Cam impingement is created by the abnormal development of the femoral head-neck junction causing what has previously been described as a 'pistol-grip deformity'. This type of deformity is characterised by varying amounts of abnormal bone on the anterior and superior femoral neck at the head-neck
106:
The concept of FAI was first described by Smith-Petersen. However, modern diagnosis and treatment of FAI was pioneered by Ganz in 2003, who initially advocated the use of an open surgical dislocation technique for treatment of intra-articular pathology. This involved the use of the 'trochanteric
482:
The cartilage lining of the socket is in the shape of an inverted horseshoe. The middle of this is termed the cotyloid fossa. Arising from the cotyloid fossa and connecting to the femoral head lies the ligamentum teres. The function of this in the adult is under debate, but in childhood the
355:
New techniques are prevalent in hip arthroscopy. There is good evidence to support the creation of a new labrum by performing a labral reconstruction if the patient has previously had a labral debridement, has an ossified labrum, or the current labrum is too small or injured for a repair.
240:
295:
referred to as the 'central compartment' of the hip, traction is released, allowing the ball of the hip to sit back snugly into its socket. The arthroscope is then moved to the 'peripheral compartment' an area still inside the hip joint itself but outside its ball and socket portion.
1065:
Nepple, Jeffrey J.; Philippon, Marc J.; Campbell, Kevin J.; Dornan, Grant J.; Jansson, Kyle S.; LaPrade, Robert F.; Wijdicks, Coen A. (2014). "The hip fluid seal—Part II: The effect of an acetabular labral tear, repair, resection, and reconstruction on hip stability to distraction".
25:
398:
Anaesthetic complications are fortunately rare, but include post-operative chest infection, urinary retention (inability to pass urine), gastrointestinal problems (constipation, nausea), heart complications (such as an abnormal rhythm), and even death.
389:
Hip arthroscopy is generally a very safe technique. However, as with all surgical procedures, there are possible pitfalls and complications. These can be divided into general complications of an operation and those specific to hip arthroscopy itself.
437:
approximation, for FAI surgery undertaken arthroscopically, 80% of patients feel their hips are improved one year after the operation, 15% feel their symptoms are unaltered while 5% may be made worse. If the procedure is being performed for early
469:(the socket). Both the ball and socket are congruous and covered with hyaline (or articular) cartilage, which allows smooth, almost frictionless gliding between the two surfaces. The edge of the acetabulum is surrounded by the
360:
involves creating a new labrum either from the patients own tissue (autograft) or from cadaver tissue (allograft). The new labrum is then anchored into position with bone anchors and the hip then goes through extensive rehab.
91:
surgeon to gain access to reliable views of increasingly smaller joint spaces. Now, there is an
International Society for Hip Arthroscopy (ISHA), comprising some of the leading hip arthroscopy specialists in the world.
307:
419:
hours without intervention. Very rarely some of this irrigation fluid can track upwards into the abdomen. Should this occur, the patient may complain of back pain immediately after surgery.
270:
Figure 5. Portal placement under direct vision. The instrument is entering the joint through the hip capsule, between the femoral head (on the left) and acetabular labrum (on the right)
645:
Botser, I. B.; Smith Jr., T. W.; Nasser, R.; Domb, B. G. (2011). "Open
Surgical Dislocation Versus Arthroscopy for Femoroacetabular Impingement: A Comparison of Clinical Outcomes".
501:"The Classic: Treatment of Malum Coxae Senilis, Old Slipped Upper Femoral Epiphysis, Intrapelvic Protrusion of the Acetabulum, and Coxa Plana by Means of Acetabuloplasty"
139:
1461:
Kelly, B. T.; Shapiro, G. S.; Digiovanni, C. W.; Buly, R. L.; Potter, H. G.; Hannafin, J. A. (2005). "Vascularity of the hip labrum: A cadaveric investigation".
311:
Figure 8.Cartilage delamination. A small area of acetabular cartilage has lifted from the underlying bone, being demonstrated by use of the arthroscopic probe
1186:
Ilizaliturri Jr, V.; Camacho-Galindo, J.; Evia
Ramirez, A.; Gonzalez Ibarra, Y.; McMillan, S.; Busconi, B. (2011). "Soft tissue pathology around the hip".
553:"Hip morphology influences the pattern of damage to the acetabular cartilage: FEMOROACETABULAR IMPINGEMENT AS a CAUSE OF EARLY OSTEOARTHRITIS OF THE HIP"
258:
Figure 4. A needle is passed into the joint, breaking the 'suction seal', and allowing further distraction of the hip joint with minimal extra traction
949:
Dienst, M.; Kusma, M.; Steimer, O.; Holzhoffer, P.; Kohn, D. (2010). "Arthroskopische
Behandlung des femoroazetabulären Cam-Impingements der Hüfte".
381:, deep gluteal syndrome and ischiofemoral impingement. Although the majority of these are newly described techniques, the results appear favorable.
1117:
Ferguson, Stephen J; Bryant, J.T; Ganz, R; Ito, K (2003). "An in vitro investigation of the acetabular labral seal in hip joint mechanics".
299:
specially designed anchors may be used. This is by no means a comprehensive list as new instruments are being developed constantly.
1550:
824:
Gedouin, J. -E.; May, O.; Bonin, N.; Nogier, A.; Boyer, T.; Sadri, H.; Villar, R. -N.; Laude, F.; French
Arthroscopy, S. (2010).
1314:"Early outcome of hip arthroscopy for femoroacetabular impingement: THE ROLE OF FEMORAL OSTEOPLASTY IN SYMPTOMATIC IMPROVEMENT"
902:"Early outcome of hip arthroscopy for femoroacetabular impingement: THE ROLE OF FEMORAL OSTEOPLASTY IN SYMPTOMATIC IMPROVEMENT"
407:
Despite being uncommon, less than 1%, the risk of infection after hip arthroscopy always present. Development of blood clots (
131:
370:
369:
The hip arthroscope may also be used to treat other conditions, which are outside the hip joint capsule. These include
680:
984:
Bhatia, S (15 Jul 2015). "Effects of
Acetabular Rim Trimming on Hip Joint Contact Pressures: How Much Is Too Much?".
246:
Figure 3. Fluoroscopic picture showing a mild amount of distraction of the hip before insertion of any instruments
143:
Figure 7. A complex labral tear. An arthroscopic probe is seen at the junction of the labrum and acetabular rim
411:) is also a risk, probably created by the slowing of blood flow in the veins as a result of reduced mobility.
96:
737:
Byrd, J. W. T.; Jones, K. S. (2004). "Traumatic rupture of the ligamentum teres as a source of hip pain".
716:
826:"Assessment of arthroscopic management of femoroacetabular impingement. A prospective multicenter study"
698:
108:
441:(wear and tear), the results are not as clear-cut, and a larger proportion may not feel benefit.
346:
320:
using high-speed motorised burrs that are similar in design to a dentist's drill (see fig. 9).
46:. The upper instrument is the arthroscope (viewing device), while the lower is the high-speed
374:
357:
449:
408:
1412:"The incidence of total hip arthroplasty after hip arthroscopy in osteoarthritic patients"
8:
1185:
378:
276:
116:
1527:
1438:
1411:
1387:
1362:
1343:
1288:
1263:
1099:
1009:
931:
798:
773:
627:
614:
601:
582:
525:
500:
280:
120:
1130:
1519:
1478:
1443:
1392:
1335:
1293:
1244:
1221:
Martin, H. D.; Shears, S. A.; Johnson, J. C.; Smathers, A. M.; Palmer, I. J. (2011).
1203:
1168:
1164:
1134:
1091:
1083:
1044:
1001:
966:
923:
882:
847:
803:
754:
662:
619:
574:
530:
471:
100:
1531:
1347:
935:
631:
1509:
1470:
1433:
1423:
1382:
1374:
1325:
1283:
1275:
1234:
1195:
1160:
1126:
1103:
1075:
1036:
1013:
993:
958:
913:
874:
837:
793:
785:
746:
654:
609:
586:
564:
520:
512:
1330:
1313:
918:
901:
1514:
1497:
1474:
1239:
1222:
750:
658:
569:
552:
1264:"Complications of Arthroscopic Femoroacetabular Impingement Treatment: A Review"
600:
Ganz, R.; Parvizi, J.; Beck, M.; Leunig, M.; Nötzli, H.; Siebenrock, K. (2003).
842:
825:
330:
115:
to heal back properly, persistent pain following the formation of scar tissue (
1378:
1279:
1199:
1079:
962:
878:
865:
Sampson, T. (2011). "Arthroscopic treatment for chondral lesions of the hip".
789:
516:
1544:
1087:
997:
772:
Tannast, M.; Goricki, D.; Beck, M.; Murphy, S. B.; Siebenrock, K. A. (2008).
155:
Table 1. A selection of hip conditions that may be treated arthroscopically.
47:
1223:"The Endoscopic Treatment of Sciatic Nerve Entrapment/Deep Gluteal Syndrome"
111:(new bone formation around the hip), nerve injuries, failure of the greater
1523:
1482:
1447:
1428:
1396:
1339:
1297:
1248:
1207:
1138:
1095:
1048:
1005:
970:
927:
886:
851:
807:
758:
666:
623:
578:
534:
1172:
135:
Figure 6. Diagram of the bony pathology of both cam and pincer impingement
1155:
Kim, Y.; Azuma, H. (1995). "The nerve endings of the acetabular labrum".
1040:
284:
87:
70:
35:
31:
1027:
Field, R. E.; Rajakulendran, K. (2011). "The Labro-Acetabular
Complex".
58:
466:
461:
is essentially a ball and socket joint. It consists of the head of the
112:
1416:
Sports
Medicine, Arthroscopy, Rehabilitation, Therapy & Technology
602:"Femoroacetabular impingement: A cause for osteoarthritis of the hip"
438:
476:
1363:"Prospective Analysis of Hip Arthroscopy with 10-year Followup"
774:"Hip Damage Occurs at the Zone of Femoroacetabular Impingement"
1064:
462:
43:
948:
1312:
Bardakos, N. V.; Vasconcelos, J. C.; Villar, R. N. (2008).
1220:
900:
Bardakos, N. V.; Vasconcelos, J. C.; Villar, R. N. (2008).
323:
1460:
39:
1311:
899:
644:
458:
75:
771:
302:
148:
labral tears and cartilage abnormalities, among others (
123:
procedure (i.e. no need to stay in hospital overnight).
830:
Orthopaedics & Traumatology: Surgery & Research
1060:
1058:
681:"Femoral-Acetabular Impingement (FAI) - Dr. Ben Petre"
1116:
823:
599:
550:
275:
The procedure is performed with the patient asleep (
1055:
551:Beck, M.; Kalhor, M.; Leunig, M.; Ganz, R. (2005).
1409:
1255:
1179:
1026:
492:
1502:Journal of Bone and Joint Surgery. British Volume
1318:Journal of Bone and Joint Surgery. British Volume
906:Journal of Bone and Joint Surgery. British Volume
557:Journal of Bone and Joint Surgery. British Volume
1542:
819:
817:
732:
730:
216:Sciatic nerve compression (piriformis syndrome)
858:
422:
191:Ligamentum teres injuries (and reconstruction)
1495:
1068:Knee Surgery, Sports Traumatology, Arthroscopy
893:
498:
1489:
1304:
1110:
814:
727:
196:Iliopsoas tendinopathy (or 'snapping psoas')
74:refers to the viewing of the interior of the
1261:
765:
393:
364:
1403:
1214:
1150:
1148:
1020:
942:
546:
544:
1454:
1367:Clinical Orthopaedics and Related Research
1354:
1268:Clinical Orthopaedics and Related Research
1157:Clinical Orthopaedics and Related Research
778:Clinical Orthopaedics and Related Research
638:
606:Clinical Orthopaedics and Related Research
505:Clinical Orthopaedics and Related Research
402:
181:Chondral (cartilage) lesions (see fig. 8)
161:Femoroacetabular impingement (see fig. 6)
24:
1513:
1437:
1427:
1386:
1360:
1329:
1287:
1238:
917:
841:
797:
736:
613:
568:
524:
1154:
1145:
717:"Hip Cartilage Injuries - Dr. Ben Petre"
593:
541:
453:Figure 1. Basic anatomy of the hip joint
448:
324:Pincer-type femoroacetabular impingement
306:
138:
130:
86:The first man to describe the use of an
1498:"The ligamentum teres of the adult hip"
1496:Bardakos, N. V.; Villar, R. N. (2009).
864:
709:
691:
673:
1543:
983:
951:Operative Orthopädie und Traumatologie
226:Direct assessment of hip replacement
176:Hip washout (for infection) or biopsy
1361:Byrd, J. W. T.; Jones, K. S. (2009).
1029:The Journal of Bone and Joint Surgery
303:Cam-type femoroacetabular impingement
986:American Journal of Sports Medicine
699:"Hip Labral Repair - Dr. Ben Petre"
95:of pathological conditions such as
13:
615:10.1097/01.blo.0000096804.78689.c2
371:greater trochanteric pain syndrome
14:
1562:
1410:Haviv, B.; O'Donnell, J. (2010).
1165:10.1097/00003086-199511000-00029
384:
263:
251:
239:
977:
340:
211:Osteoarthritis (controversial)
1551:Orthopedic surgical procedures
499:Smith-Petersen, M. N. (2008).
126:
1:
1331:10.1302/0301-620X.90B12.21012
1131:10.1016/s0021-9290(02)00365-2
919:10.1302/0301-620X.90B12.21012
486:
171:Loose / foreign body removal
1515:10.1302/0301-620X.91B1.21421
1475:10.1016/j.arthro.2004.09.016
1262:Ilizaliturri, V. M. (2008).
1240:10.1016/j.arthro.2010.07.008
751:10.1016/j.arthro.2004.01.025
659:10.1016/j.arthro.2010.11.008
570:10.1302/0301-620X.87B7.15203
423:Postoperative rehabilitation
232:
97:femoroacetabular impingement
50:used for reshaping the bone.
7:
201:Trochanteric pain syndrome
10:
1567:
1188:Clinics in Sports Medicine
867:Clinics in Sports Medicine
843:10.1016/j.otsr.2010.08.002
444:
431:
344:
221:Ischiofemoral impingement
186:Osteochondritis dissecans
166:Labral tears (see fig. 7)
81:
1379:10.1007/s11999-009-0841-7
1280:10.1007/s11999-008-0618-4
1200:10.1016/j.csm.2010.12.009
1080:10.1007/s00167-014-2875-y
963:10.1007/s00064-010-3003-5
879:10.1016/j.csm.2010.12.012
790:10.1007/s11999-007-0061-y
517:10.1007/s11999-008-0670-0
394:Anaesthetic complications
365:Extra-articular syndromes
206:Snapping iliotibial band
55:
23:
18:
1125:(2). Elsevier: 171–178.
998:10.1177/0363546515590400
375:snapping iliotibial band
109:heterotopic ossification
1119:Journal of Biomechanics
403:Operative complications
99:(FAI) and tears of the
1429:10.1186/1758-2555-2-18
454:
347:Acetabular labrum tear
312:
144:
136:
452:
358:Labral reconstruction
310:
142:
134:
1041:10.2106/JBJS.J.01710
409:deep-vein thrombosis
465:(the ball) and the
379:piriformis syndrome
277:general anaesthetic
455:
313:
281:spinal anaesthesia
145:
137:
1324:(12): 1570–1575.
912:(12): 1570–1575.
472:acetabular labrum
230:
229:
101:acetabular labrum
66:
65:
1558:
1536:
1535:
1517:
1493:
1487:
1486:
1458:
1452:
1451:
1441:
1431:
1407:
1401:
1400:
1390:
1358:
1352:
1351:
1333:
1308:
1302:
1301:
1291:
1259:
1253:
1252:
1242:
1218:
1212:
1211:
1183:
1177:
1176:
1159:(320): 176–181.
1152:
1143:
1142:
1114:
1108:
1107:
1062:
1053:
1052:
1024:
1018:
1017:
981:
975:
974:
946:
940:
939:
921:
897:
891:
890:
862:
856:
855:
845:
821:
812:
811:
801:
769:
763:
762:
734:
725:
724:
713:
707:
706:
695:
689:
688:
677:
671:
670:
642:
636:
635:
617:
608:(417): 112–120.
597:
591:
590:
572:
563:(7): 1012–1018.
548:
539:
538:
528:
496:
267:
255:
243:
158:
157:
76:acetabulofemoral
59:edit on Wikidata
34:image during an
28:
16:
15:
1566:
1565:
1561:
1560:
1559:
1557:
1556:
1555:
1541:
1540:
1539:
1494:
1490:
1459:
1455:
1408:
1404:
1359:
1355:
1309:
1305:
1260:
1256:
1219:
1215:
1184:
1180:
1153:
1146:
1115:
1111:
1063:
1056:
1025:
1021:
982:
978:
947:
943:
898:
894:
863:
859:
822:
815:
770:
766:
735:
728:
715:
714:
710:
697:
696:
692:
679:
678:
674:
643:
639:
598:
594:
549:
542:
497:
493:
489:
447:
434:
425:
405:
396:
387:
367:
349:
343:
326:
305:
271:
268:
259:
256:
247:
244:
235:
129:
84:
62:
51:
38:resection of a
30:Intraoperative
19:Hip arthroscopy
12:
11:
5:
1564:
1554:
1553:
1538:
1537:
1488:
1453:
1402:
1373:(3): 741–746.
1353:
1303:
1274:(3): 760–768.
1254:
1233:(2): 172–181.
1213:
1194:(2): 391–415.
1178:
1144:
1109:
1074:(4): 730–736.
1054:
1019:
992:(9): 2138–45.
976:
941:
892:
873:(2): 331–348.
857:
836:(8): S59–S67.
813:
784:(2): 273–280.
764:
745:(4): 385–391.
726:
708:
690:
672:
653:(2): 270–278.
637:
592:
540:
511:(3): 608–615.
490:
488:
485:
446:
443:
433:
430:
424:
421:
404:
401:
395:
392:
386:
383:
366:
363:
345:Main article:
342:
339:
331:osteoarthritis
325:
322:
304:
301:
273:
272:
269:
262:
260:
257:
250:
248:
245:
238:
234:
231:
228:
227:
223:
222:
218:
217:
213:
212:
208:
207:
203:
202:
198:
197:
193:
192:
188:
187:
183:
182:
178:
177:
173:
172:
168:
167:
163:
162:
128:
125:
83:
80:
64:
63:
56:
53:
52:
29:
21:
20:
9:
6:
4:
3:
2:
1563:
1552:
1549:
1548:
1546:
1533:
1529:
1525:
1521:
1516:
1511:
1507:
1503:
1499:
1492:
1484:
1480:
1476:
1472:
1468:
1464:
1457:
1449:
1445:
1440:
1435:
1430:
1425:
1421:
1417:
1413:
1406:
1398:
1394:
1389:
1384:
1380:
1376:
1372:
1368:
1364:
1357:
1349:
1345:
1341:
1337:
1332:
1327:
1323:
1319:
1315:
1307:
1299:
1295:
1290:
1285:
1281:
1277:
1273:
1269:
1265:
1258:
1250:
1246:
1241:
1236:
1232:
1228:
1224:
1217:
1209:
1205:
1201:
1197:
1193:
1189:
1182:
1174:
1170:
1166:
1162:
1158:
1151:
1149:
1140:
1136:
1132:
1128:
1124:
1120:
1113:
1105:
1101:
1097:
1093:
1089:
1085:
1081:
1077:
1073:
1069:
1061:
1059:
1050:
1046:
1042:
1038:
1034:
1030:
1023:
1015:
1011:
1007:
1003:
999:
995:
991:
987:
980:
972:
968:
964:
960:
956:
952:
945:
937:
933:
929:
925:
920:
915:
911:
907:
903:
896:
888:
884:
880:
876:
872:
868:
861:
853:
849:
844:
839:
835:
831:
827:
820:
818:
809:
805:
800:
795:
791:
787:
783:
779:
775:
768:
760:
756:
752:
748:
744:
740:
733:
731:
722:
718:
712:
704:
700:
694:
686:
682:
676:
668:
664:
660:
656:
652:
648:
641:
633:
629:
625:
621:
616:
611:
607:
603:
596:
588:
584:
580:
576:
571:
566:
562:
558:
554:
547:
545:
536:
532:
527:
522:
518:
514:
510:
506:
502:
495:
491:
484:
480:
478:
474:
473:
468:
464:
460:
451:
442:
440:
429:
420:
416:
412:
410:
400:
391:
385:Complications
382:
380:
376:
372:
362:
359:
353:
348:
338:
334:
332:
321:
317:
309:
300:
296:
292:
288:
286:
282:
278:
266:
261:
254:
249:
242:
237:
236:
225:
224:
220:
219:
215:
214:
210:
209:
205:
204:
200:
199:
195:
194:
190:
189:
185:
184:
180:
179:
175:
174:
170:
169:
165:
164:
160:
159:
156:
153:
151:
141:
133:
124:
122:
118:
114:
110:
104:
102:
98:
92:
89:
79:
77:
73:
72:
60:
54:
49:
45:
41:
37:
33:
27:
22:
17:
1505:
1501:
1491:
1466:
1462:
1456:
1419:
1415:
1405:
1370:
1366:
1356:
1321:
1317:
1306:
1271:
1267:
1257:
1230:
1226:
1216:
1191:
1187:
1181:
1156:
1122:
1118:
1112:
1071:
1067:
1032:
1028:
1022:
989:
985:
979:
957:(1): 29–43.
954:
950:
944:
909:
905:
895:
870:
866:
860:
833:
829:
781:
777:
767:
742:
738:
720:
711:
702:
693:
684:
675:
650:
646:
640:
605:
595:
560:
556:
508:
504:
494:
481:
470:
456:
435:
426:
417:
413:
406:
397:
388:
368:
354:
350:
341:Labral tears
335:
327:
318:
314:
297:
293:
289:
274:
154:
149:
146:
105:
93:
85:
68:
67:
36:arthroscopic
32:fluoroscopic
1508:(1): 8–15.
1469:(1): 3–11.
1463:Arthroscopy
1227:Arthroscopy
739:Arthroscopy
721:drpetre.com
703:drpetre.com
685:drpetre.com
647:Arthroscopy
285:fluoroscopy
279:) or under
150:see Table 1
127:Indications
88:arthroscope
71:arthroscopy
487:References
467:acetabulum
121:outpatient
113:trochanter
40:cam lesion
1088:0942-2056
1035:: 22–27.
439:arthritis
233:Technique
117:adhesions
1545:Category
1532:18094438
1524:19091998
1483:15650660
1448:20670440
1397:19381742
1348:16486786
1340:19043126
1298:19018604
1249:21071168
1208:21419963
1139:12547354
1096:24509878
1049:21543684
1006:26180260
971:20349168
936:16486786
928:19043126
887:21419959
852:21035415
808:18196406
759:15067278
667:21266277
632:37330685
624:14646708
579:15972923
535:19089521
477:synovium
373:(GTPS),
1439:2924275
1388:2816779
1289:2635434
1173:7586824
1104:9258547
1014:1172435
799:2505146
587:7844494
526:2635442
445:Anatomy
432:Results
82:History
42:of the
1530:
1522:
1481:
1446:
1436:
1422:: 18.
1395:
1385:
1346:
1338:
1296:
1286:
1247:
1206:
1171:
1137:
1102:
1094:
1086:
1047:
1012:
1004:
969:
934:
926:
885:
850:
806:
796:
757:
665:
630:
622:
585:
577:
533:
523:
1528:S2CID
1344:S2CID
1310:</
1100:S2CID
1010:S2CID
932:S2CID
628:S2CID
583:S2CID
463:femur
57:[
44:femur
1520:PMID
1506:91-B
1479:PMID
1444:PMID
1393:PMID
1336:PMID
1322:90-B
1294:PMID
1245:PMID
1204:PMID
1169:PMID
1135:PMID
1092:PMID
1084:ISSN
1045:PMID
1002:PMID
967:PMID
924:PMID
910:90-B
883:PMID
848:PMID
804:PMID
755:PMID
663:PMID
620:PMID
575:PMID
561:87-B
531:PMID
457:The
69:Hip
48:burr
1510:doi
1471:doi
1434:PMC
1424:doi
1383:PMC
1375:doi
1371:468
1326:doi
1284:PMC
1276:doi
1272:467
1235:doi
1196:doi
1161:doi
1127:doi
1076:doi
1037:doi
994:doi
959:doi
914:doi
875:doi
838:doi
794:PMC
786:doi
782:466
747:doi
655:doi
610:doi
565:doi
521:PMC
513:doi
509:467
459:hip
152:).
1547::
1526:.
1518:.
1504:.
1500:.
1477:.
1467:21
1465:.
1442:.
1432:.
1418:.
1414:.
1391:.
1381:.
1369:.
1365:.
1342:.
1334:.
1320:.
1316:.
1292:.
1282:.
1270:.
1266:.
1243:.
1231:27
1229:.
1225:.
1202:.
1192:30
1190:.
1167:.
1147:^
1133:.
1123:36
1121:.
1098:.
1090:.
1082:.
1072:22
1070:.
1057:^
1043:.
1033:93
1031:.
1008:.
1000:.
990:43
988:.
965:.
955:22
953:.
930:.
922:.
908:.
904:.
881:.
871:30
869:.
846:.
834:96
832:.
828:.
816:^
802:.
792:.
780:.
776:.
753:.
743:20
741:.
729:^
719:.
701:.
683:.
661:.
651:27
649:.
626:.
618:.
604:.
581:.
573:.
559:.
555:.
543:^
529:.
519:.
507:.
503:.
377:,
333:.
103:.
1534:.
1512::
1485:.
1473::
1450:.
1426::
1420:2
1399:.
1377::
1350:.
1328::
1300:.
1278::
1251:.
1237::
1210:.
1198::
1175:.
1163::
1141:.
1129::
1106:.
1078::
1051:.
1039::
1016:.
996::
973:.
961::
938:.
916::
889:.
877::
854:.
840::
810:.
788::
761:.
749::
723:.
705:.
687:.
669:.
657::
634:.
612::
589:.
567::
537:.
515::
61:]
Text is available under the Creative Commons Attribution-ShareAlike License. Additional terms may apply.